Well, well, well. I did say I wouldn’t update this blog again until I had neutrophils, and now I have NEUTROPHILS!!! As I’m sure you’re already well aware if you’re reading this, because I have shouted it emphatically at anyone and everyone within physical and digital hearing range.
Not only have I had neutrophils for a month now, but since my beautiful sweet little neuts returned my count has remained above 1 the entire time, and at its highest it was 17 😱. A normal neutrophil count is between 1.5 – 8, so 17 was fiercely celebrated but a bit extreme. What was also extreme was my bone pain at this time, I had been warned that having bone marrow swelling from all of the new cell activity would be painful but sheeeesh.
I have said this a thousand times to anyone that will listen, but I am still in shock that my neutrophils came back so rapidly, after so long of NOTHING. Bizarrely in the first few days of my hospital admission, my neut count crept up to 0.07 before plummeting back to 0 for the next 7 weeks. Haematology didn’t want to discharge me until my ANC was 1.5, so by my calculations, once daclizumab was cleared from my system/the treatment kicked in it would take me at least a further 2 months to reach a healthy neutrophil count. And that was only if the damage was reversible/drugs would work.

Because there was no precedent for what happened to me, the doctors had no idea what to do. The theory was that daclizumab (my MS treatment) had interacted with my CVID (Common Variable Immune Deficiency) and shut down my neutrophil production, but this was just the most likely scenario and none of the doctors could confirm with certainty that this was actually what had happened. Daclizumab had only been TGA approved for use in RRMS for less than a year so literature was lacking, and from what I understand the incidence of people with both MS and CVID is extremely low (MS is approx 1:1000, CVID is approx 1:30,000). Haematology came in on numerous occasions and just flat out told me “we honestly have no idea what to do with you.” Immunology told me that they were trying everything they could and were researching like mad but had no idea if I would ever recover. And at the height of the infection I caught whilst neutropenic when I was looking for reassurance and asked a doctor from the Infectious Diseases department if I was going to die, all he could offer was “I really hope not.”
Most of my 8 weeks in hospital has blurred into one long horrific day, but August 8 stands out as the day I literally got my life back. It started out like any other day, which was basically me trying to make myself look as presentable and healthy as possible so the doctors would approve me for day leave (essentially I just put clothes on and brushed my hair, which I was too sick to do for the first month so this was a big improvement 😂).
I was sitting on the bed trying to make myself look nonchalant and full of energy when the resident came in and told me that incredibly my neutrophil count from the day before had come back as 0.07. 0.07 was amazing. I could have cried. Then the consultant came in and told me that the count was actually 0.7. I did cry. The haematologists wanted to check my films with their own eyes before we celebrated, so off they went to the lab, and came back shortly after to confirm that my blood was ABUNDANT with fluffy little white cells. Even the consultant from my haem team who had just rotated off from ward duty came up to tell me he wanted to crack a bottle of champagne. After spending 7 weeks thinking I was more than likely going to die, the rush of elation and relief was indescribable. I went on day leave but missed a call from the hospital shortly after. They left a voicemail telling me that my neutrophil count from my bloods taken that morning was 3.9. I lay in my bed and listened to that voicemail 20 times.
In the space of 24 hours, I had gone from being a patient that ticked every single box in the highest risk category to completely normal. We ripped up the sign on my door telling hospital staff and visitors to wear masks around me, we stopped the GCSF injections that were stimulating my bone marrow, I started eating fruit and vegetables that didn’t need to be peeled (bacteria risk) and I threw out all my Dettol (just kidding, I’m not that reckless).
Even my haematologists seemed surprised at my neutrophils’ dramatic reappearance, but reasoned that they had been flogging my body with every drug imaginable and it had all finally kicked in. For the first time since I was admitted, a planned discharge date went up on the board in my room. It was one week away, and in that time we’d make sure my neutrophils stayed stable off the GCSF, and start tinkering with the dosages of my other meds.
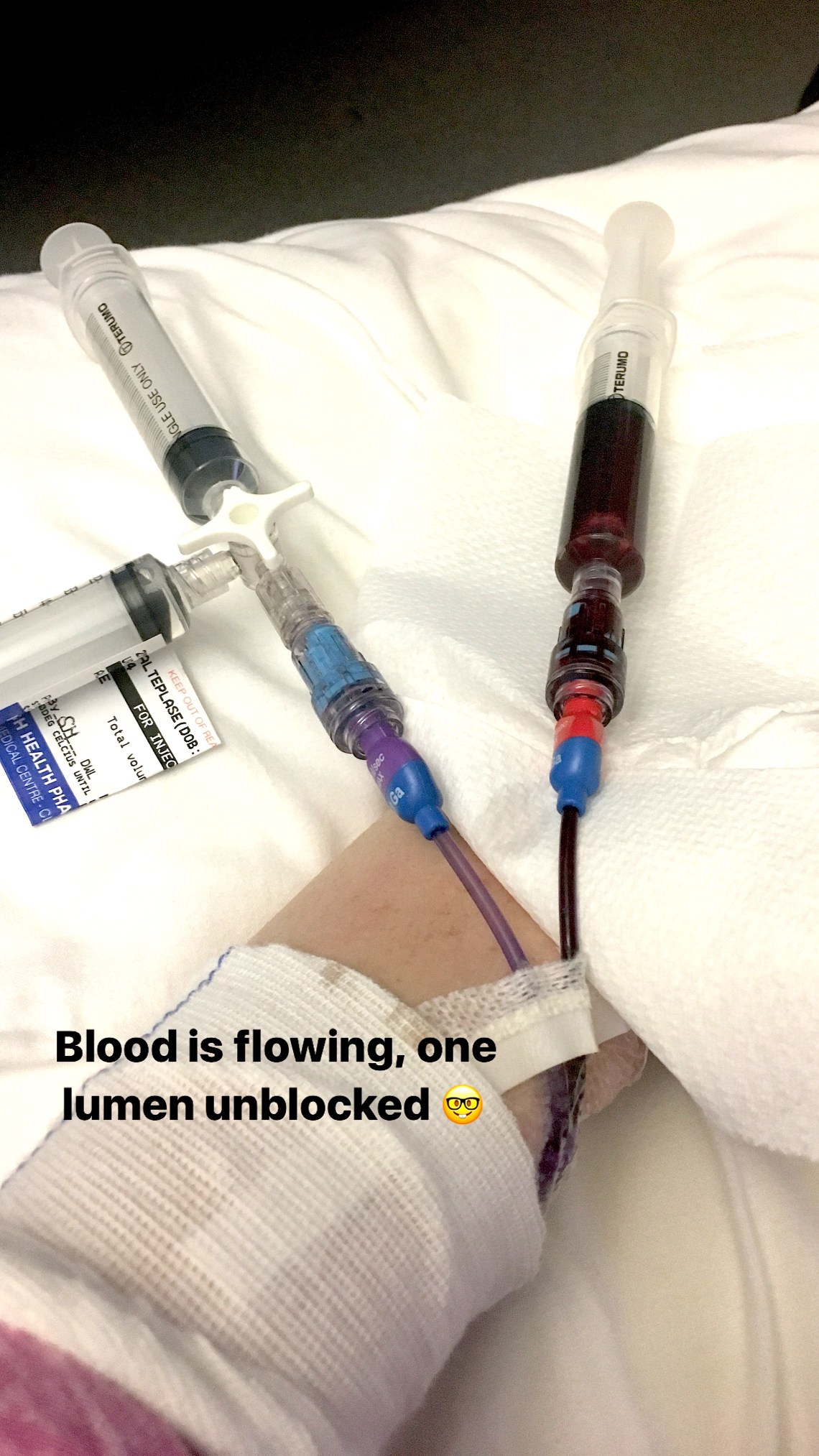
Of course nothing is ever that simple with me, and whilst my white blood cells were behaving beautifully, in the lead up to discharge I was extremely tachycardic and my haemoglobin was dropping. The haematologists had no explanation for my haemoglobin levels except that maybe my bone marrow was still in a bit of a slump. We knew that it was likely the same thing causing my tachycardia and anaemia, and the haematologists were worried that it might be an infection that my immunosuppression meant I wasn’t showing any other symptoms for. We pulled my PICC line out early in case that was the infection source but the tip of the PICC was sent for testing and didn’t grow anything.

By the time it came to my planned day of discharge however the new thinking was that I either had a blood clot in my lungs or a slow internal bleed 😑. By now my haemoglobin had dropped to 72, so I was given another blood transfusion. Haematology weren’t overly concerned by the possibility of an internal bleed, but they were worried about the possibility of a blood clot. So I was sent down to nuclear medicine because I haven’t had enough radiation exposure 💁
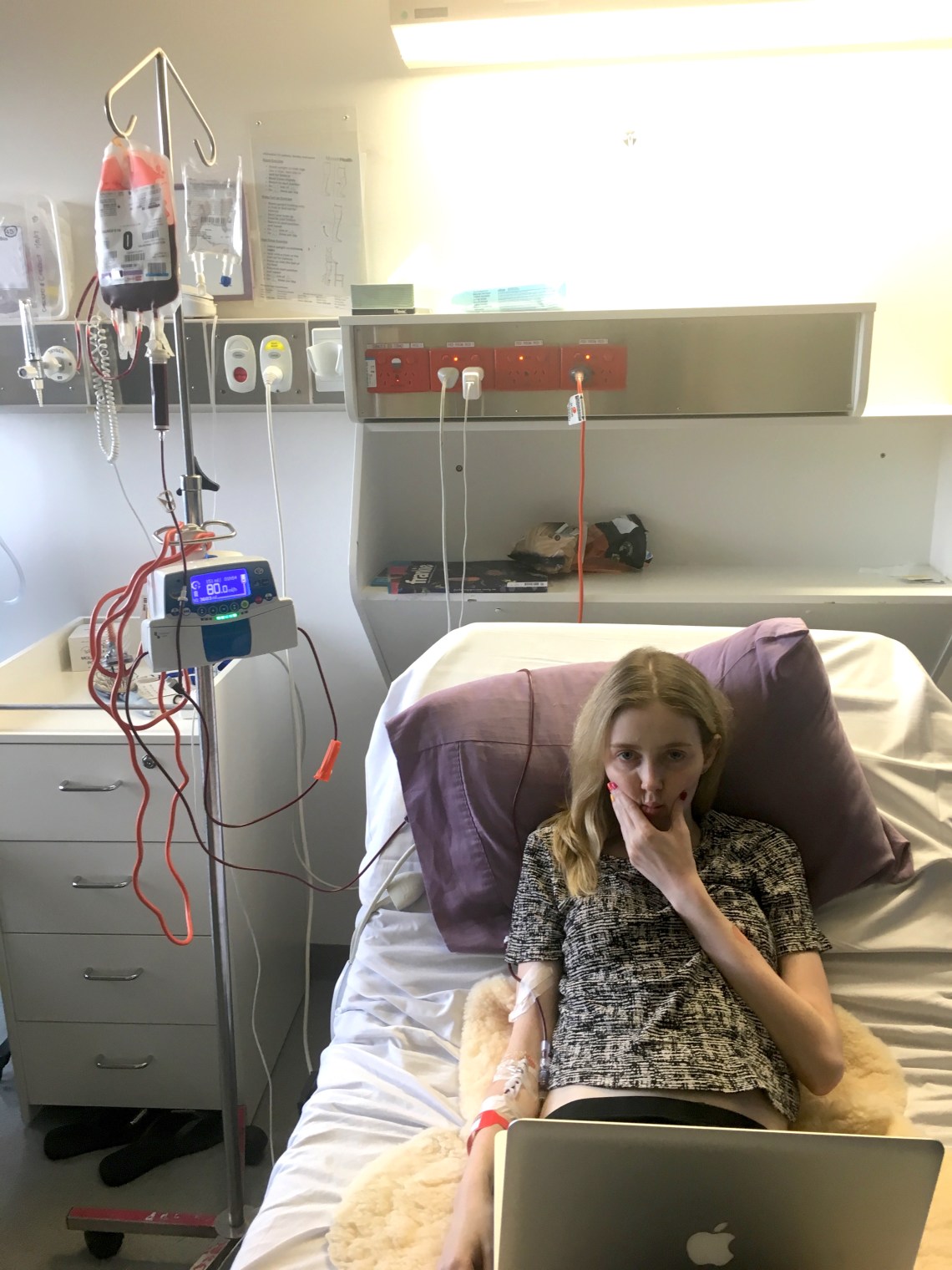
After more x-rays looking for infection in my body, I had 2 SPECT scans. For the first scan I had to breathe in a radioactive gas, and then for the second scan I was injected with a radioactive dye. Both scans were of my lungs, and compared where the radioactive gas was able to travel with where the dye went. If there were discrepancies then that meant I had a clot.

By the time I got back to the ward it was nearly 7pm and I had completely given up on discharge that day. But then one of my doctors came to see me – the scans confirmed I had no blood clot and I was good to go home!!!!

After being in hospital so long it was a strange feeling being discharged and almost anticlimactic. I was relieved, overwhelmed, sad, and scared that something would happen and I would die without constant observation.
I hadn’t had a good sleep the entire time I was in hospital, be it from the drug-induced insomnia, ward noises (the haematology ward is the LOUDEST ward I have ever been in and there seems to be a lot of MET calls – as I can attest to) or being woken up in the middle of the night for IV meds or bloods. I slept for a full 7 hours in my bed that night which was THE GREATEST. But when I woke up my heart was racing. There’s not too much normal about waking up with a heart rate of 130. I was starting to really freak out about my potential internal bleed. So it was nice to find out that I didn’t have one, and that the symptoms were not my body’s fault for once!
I went to see my gastroenterologist that day who took one look at my extensive drug chart and said she was going to have a word with haematology. I went back to Monash the day after for my methotrexate and IVIG and had my rather sheepish looking haem team come to let me know that my gastro had pointed out I was still on Dapsone as a prophylactic – a drug they’d overlooked on my chart. They ran a few tests on my blood and it turned out not only was Dapsone causing haemolysis (destruction of my red blood cells), but it was also causing methomoglobinemia which meant that the little amount of haemoglobin I did have wasn’t able to properly deliver oxygen around my body. Noooooo wonder I felt like shit. So we unceremoniously kicked Dapsone to the curb so it could hang out with Zinbryta (and Gilenya! and Tecfidera!) in the ‘drugs that are allowed nowhere near Morgan’s blood’ club.
Now that both my neutrophils and haemoglobin are stable, I am sloooooowly weaning off prednisolone but will likely stay on methotrexate for a couple of years. MTX seems to be some kind of wonder drug in that it is also good for my MS and mysterious “looks like coeliac but isn’t coeliac” gut issues, so I am happy to stay on it, especially whilst my body is healing and reconditioning.

In terms of nutrition, I am now able to eat again like a normal person and am putting weight on 🙏🙏🙏 At my lowest in hospital I weighed 42kg, so I had a feeding tube put down my nose a second time with the idea that I would eat normally throughout the day and each night the tube would deliver me an extra 1000 calories that my body so desperately needed. I have barely any memory of the first tube I had during my admission because I was so unwell and barely lucid at that point, but I definitely could not tolerate the second tube. I was in a lot of pain and threw up everything I was fed so the tube lasted an entire 24 hours before it was pulled out.

The clinical nutrition doctors were pretty unimpressed and threatened to put a PEG tube in (a tube surgically placed into the stomach through the abdomen 😱) but haematology wouldn’t let anyone operate on me without neutrophils (hence why I have also had to wait for surgery on my ear for so long). Now that I am no longer neutropenic my gastro floated the option of a PEG tube again last week, but I laughed and shouted NO, so am diligently consuming all the fat shakes, protein supplements and chocolate (life is tough) that I can.

My health is a full time job at the moment and I have hospital appointments/treatment (methotrexate/IVIG) 3 or 4 days each week, but this will decrease over the next couple of months and I’ll be able to go back to work 💰. The Walter and Eliza Hall Institute is currently sequencing my exome in the hope that we’ll find the defective gene in my immune system for which I could potentially start treatment to correct.

I used to think of my health as the solar system. MS was the big bad sun and all of my comorbidities were planets in orbit around the MS. But now I’m starting to think MS is actually just a planet, and CVID is the real sun. MS definitely takes the planetary cake as big ol’ Jupiter, but CVID is the bastard who not only has given me an immune system deficient in antibodies, but an immune system that when confronted likes to attack and shut down various functions in my body as it sees fit. To be fair, CVID was more like a star in a distant galaxy for the first 2 decades of my life, so much so that I couldn’t see it and had no idea it existed. It wasn’t until I was 20 and began immunotherapy for my MS that the CVID became enraged. When I was diagnosed with MS I had 1 specialist – a neurologist. 4 years of immunotherapy combined with CVID later and my tally of specialist teams has hit 9 😳. If it ends in ‘-ologist’, I probably have one.
It feels outrageous that there is so much wrong with my body and the amount of medical intervention I require to stay alive, and I felt pretty bloody shit about it when I was in hospital, but I am reasonably adjusted to the fact that this is the hand I’ve been dealt and I’m living my best life. I do panic about my future and the fact that I’ve been through so much and am only 24 – there’s so many years left of my life (hopefully) for things to go wrong in! What else will happen before I turn 30! But I think my GP put it best this week when we were joking that I excel at getting sick and she said, “but you’re also incredibly good at getting better.”
This post is pretty long now and I haven’t even touched on what’s happening with my MS or my melanoma! So I will leave that for another blog post. Thanks for reading until the end and for coming along on the ride with me.
Morgan xxx

2 thoughts on “~ Neutrophilicious ~”